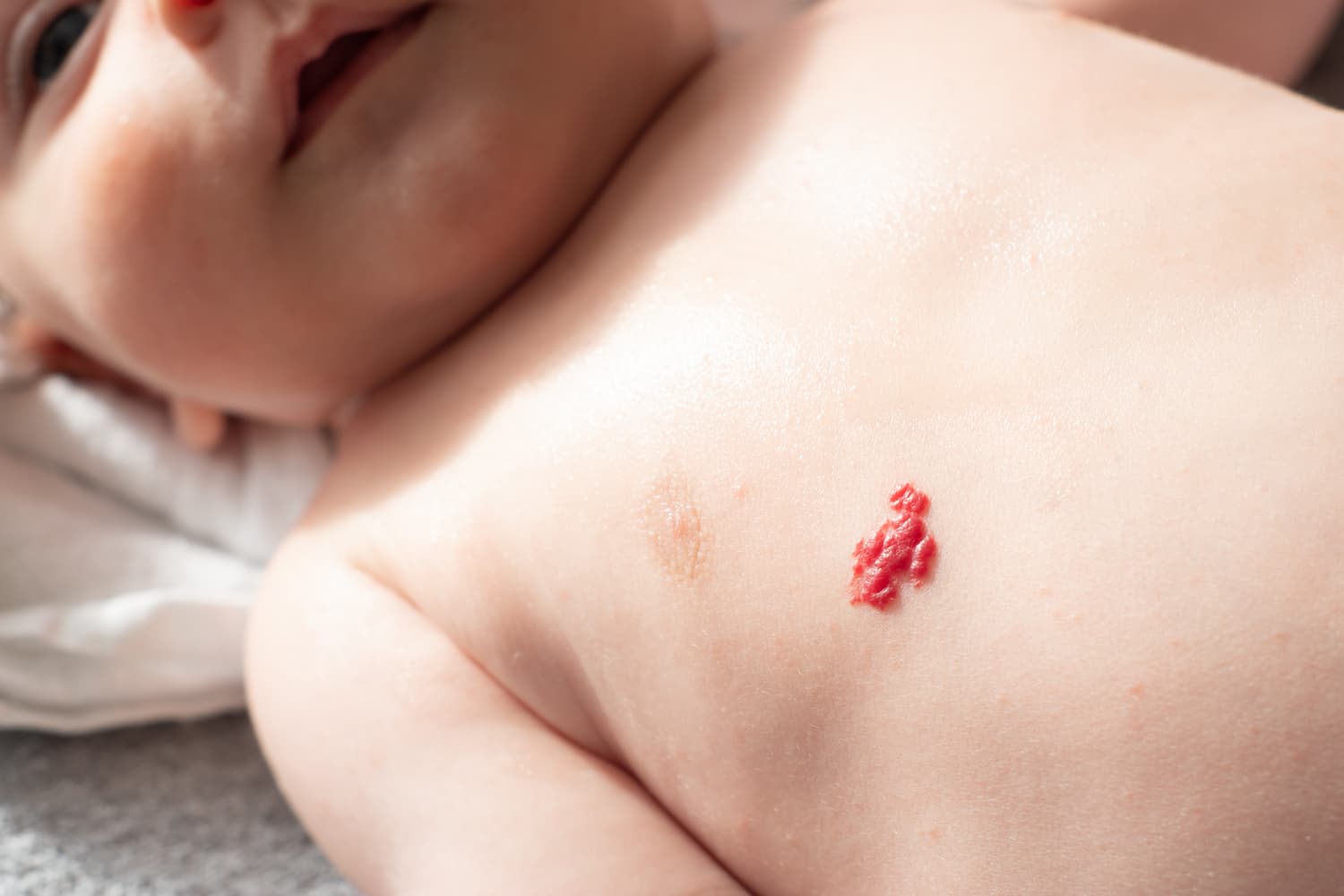
What is a haemangioma of the skin?
A ‘haemangioma’ (Greek for blood-vessel-growth) of Infancy is a benign (non-cancerous) overgrowth of blood vessel cells in the skin (cutaneous blood vessels), that is self-limiting (will stop growing without treatment).
The term ‘strawberry naevus’ or ‘strawberry haemangioma’ is used for a haemangioma that looks similar to a strawberry.
Are haemangiomas of Infancy hereditary?
Haemangiomas of infancy do not usually run in families but may rarely be inherited. They are relatively common, affecting about 5% (1 in 20) of babies. They are not contagious or cancerous.
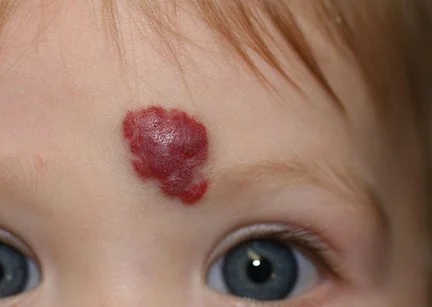
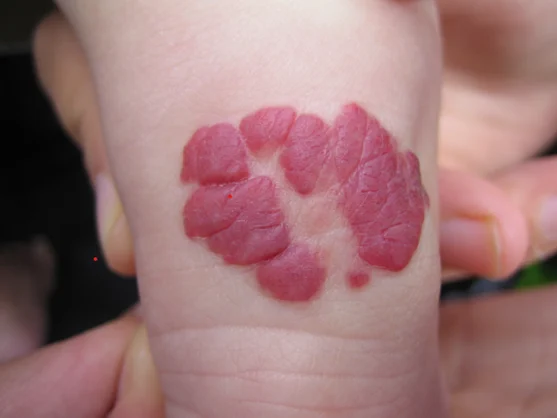
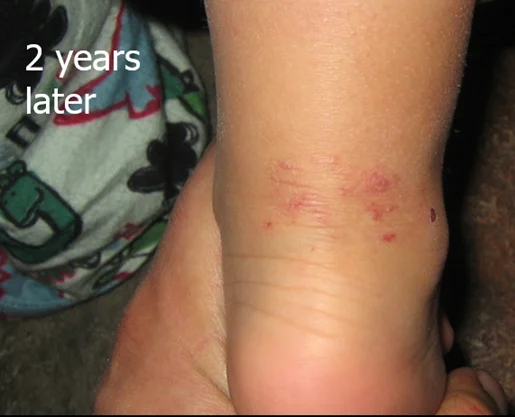
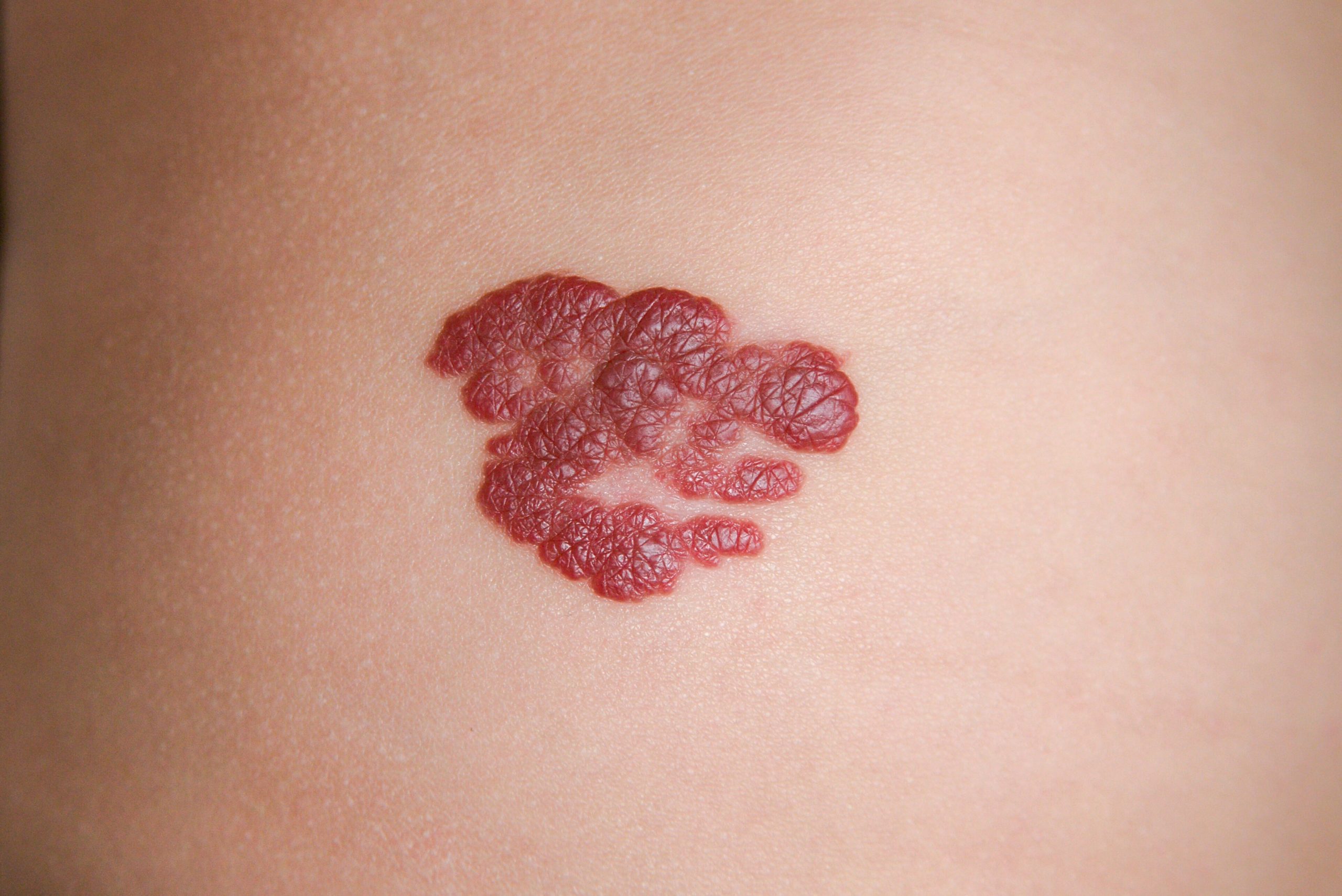
What do haemangiomas of Infancy look like?
A small red mark or swelling may be visible at birth or develop during the first weeks of life. Those with a deeper component appear as a swelling underneath the skin and may have a bluish colour. The appearance often changes rapidly during early life, usually over the first 3 months and most stop growing at about 5 months. Further change is usually slower, however they may keep growing for up to 18 months.
After this, they undergo ‘regression’, also called ‘involution’. This is the process by which the haemangioma subsequently shrinks in size, which can take from 3 to 10 years.
When a haemangioma shrinks, there may be no visible mark left behind. Some may resolve with residual blood vessels visible. Others may leave a scar (particularly if there has been ulceration of the haemangioma), a pale area of skin or an area of loose skin or thickened tissue.
Symptoms of haemangiomas of the skin
Most haemangiomas do not cause any symptoms, but can be alarming to parents and carers, especially during the phase of rapid growth. Rarely the skin over the haemangioma breaks down (ulcerates), most often in the nappy area. This can be painful. Bleeding of the ulcerated skin may occur, but this is rarely severe and usually stops with application of pressure.
Haemangiomas near the nose or mouth may cause breathing or feeding problems. Haemangiomas growing too close to the eye may interfere with the development of normal vision, especially if the eye is closed due to the swelling or if the swelling is pressing on the eye. In this case, referral to an Eye Specialist (Ophthalmologist) may be organised.
How is a haemangioma of infancy of the skin diagnosed?
The diagnosis can be made by the appearance of the haemangioma and the history of rapid growth followed by slow regression. Sometimes scans will be organised to help confirm the diagnosis or to get further information about the extent of the haemangioma, for example if it is near the eye or affecting internal organs. For deeper or less typical lesions, a biopsy (skin or tissue sample) may be required to confirm the diagnosis.
Children with haemangiomas over the midline of the lower back may require screening for underlying abnormalities of the spinal cord, inner organs and genitalia.
Deep infantile haemangiomas or segmental haemangiomas are routinely investigated with ultrasound scanning. An ultrasound scan is also often performed when there is uncertainty about the diagnosis or whether underlying tissues are affected. This is likely to involve referral to specialist teams including Paediatricians.
What are ulcerated haemangiomas?
Haemangiomas can form a painful open sore or ulcer. It’s important to visit your GP if this happens, because ulcers can become infected and might need treatment with antibiotics.
Haemangiomas around the mouth, in the nappy area or in natural folds of skin, such as the armpit, ear and neck, are most likely to become ulcerated, because the skin rubbing together causes friction.
The nappy can rub haemangiomas in the nappy area – contact with stool or urine makes the ulcer more painful.
If the child’s haemangioma develops an ulcer, it will need special attention until it heals.
- Wash the area twice a day, preferably in a bath or by pouring water over the area, and leave it to dry naturally
- Once the area is dry, cover the whole haemangioma with a non-sticky dressing (available on prescription from GPs)
Can haemangiomas of infancy be cured?
Most haemangiomas will gradually shrink or even fully disappear without leaving an obvious mark. Although many small haemangiomas clear up completely, with or without treatment, some permanent skin change can remain.

Treatments for haemangiomas of infancy
Most haemangiomas do not require treatment except in the following situations:
- If the haemangioma is particularly large or affects areas where resolution may be incomplete such as around the nose, lips or ears.
- If the haemangioma is ulcerating (the surface of the skin is broken)
- If the haemangioma is interfering with important functions such as feeding or breathing or the development of senses: e.g. hearing or vision.
For haemangiomas that are still growing, topical or oral treatments are most often used. Drugs called beta-blockers shrink blood vessels and can be used as a topical treatment or as an oral medicine.
Topical solution
A topical solution or gel applied directly to the haemangioma
Timolol can be applied as a solution or gel to the haemangioma. It has been proven to be safe and effective, especially for more superficial lesions
Medicines
Propranolol given by mouth is now the first choice to treat haemangiomas at important anatomical sites such as around the eyes or mouth. Heart rate, blood pressure and blood sugar need to be monitored during treatment. Common side effects include constipation, diarrhoea, cold arms and legs and sleep-disturbance.
Because propranolol can lower the blood sugar, it should be given during the day around feeding time and discontinued if the child is unwell. Almost all haemangiomas respond to propranolol and treatment usually lasts for 6 to 12 months.
Steroid creams, injections or tablets were frequently used before the discovery of the benefits of propranolol but are now less commonly used. Steroids may be used for children who cannot be given propranolol due to possible side effects.
Laser therapy
An ulcerating haemangioma needs additional treatment with non-adherent dressings and pain relief. Laser therapy can be useful to treat ulcerated lesions. Antibiotic ointment or medicine may also be required if infection is suspected.
After the haemangioma has stopped shrinking, laser treatment of remaining redness can sometimes be useful. In adults, usually no anaesthetic is required.
However, laser treatment in children, may require use of a general anaesthetic as laser treatment can be painful. After treatment, there is dark purple bruising in the treated area. Other possible temporary side effects include blistering, crusting and rarely, scarring may occur.
Surgery
After the haemangioma has stopped shrinking, surgical removal of excess tissue can sometimes be useful.
Surgical treatment of haemangiomas will leave a scar and is therefore not advised for uncomplicated haemangiomas, which may resolve without leaving a mark. Surgery may rarely be required to treat ulceration, obstruction or residual skin deformity caused by a haemangioma.
Cover-up makeup can be useful to cover skin discolouration. The Charity ‘Changing Faces’ may offer camouflage advice in your area (see below for further information).
Further information about a haemangioma of infancy
Download MySkinDoctor today
Organisations for Further Support:
Birthmark Support Group
Email: info@birthmarksupportgroup.org.uk
Website: www.birthmarksupportgroup.org.uk
Changing Faces
Tel: 0300 012 0275 (for support and advice)
Tel: 0300 012 0276 (for the Skin Camouflage Service)
Email: skincam@changingfaces.org.uk
Web: www.changingfaces.org.uk
British Association of Skin Camouflage (NHS and private practice)
Tel: 01254 703 107
Email: info@skin-camouflage.net
Web: www.skin-camouflage.net