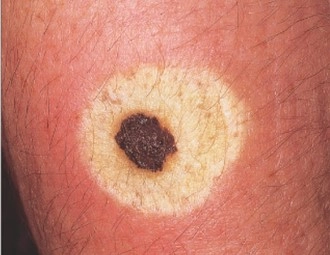
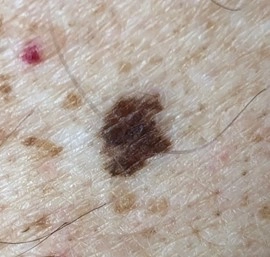
What is melanocytic naevi?
A melanocytic naevus is the medical term for a mole. The word ‘melanocytic’ means that they are made up of the cells situated deeper in the skin (melanocytes) which produce the dark pigment (melanin) that gives the skin its colour. Melanocytes can cluster together to form a clear-coloured skin lesion, or a pigmented lesion depending on how much melanin they produce. In other words, moles are benign (harmless) groups of melanocytes.
Some moles (congenital melanocytic naevi) are present at birth. Most develop during childhood and early adult life (acquired melanocytic naevi). Almost everyone has moles. Many people have between 30 and 50, or more. Many spontaneously disappear later in adult life. Moles can be found anywhere on the skin, including on the hands and feet, genitals, eyes and scalp. Most people who develop moles do not develop skin cancer.
What are the symptoms
of melanocytic naevi?
Usually there are no symptoms, but they can occasionally itch or become sore if traumatised. If these changes are persistent, lasting several weeks, they may need a specialist review. Some people do not like the appearance of their moles. Raised moles may catch on things.
Those that are present at birth (congenital melanocytic naevi) are seldom less than 1 cm in diameter but can be much larger. They grow in proportion with you as you grow. They are dark and tend to become more raised and hairier with age.
There are three main types of acquired melanocytic naevi:
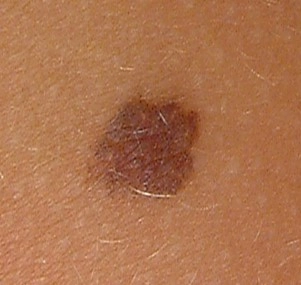
- Junctional melanocytic naevi are flat, and usually circular. Their colour is usually even, and ranges from mid to dark brown.
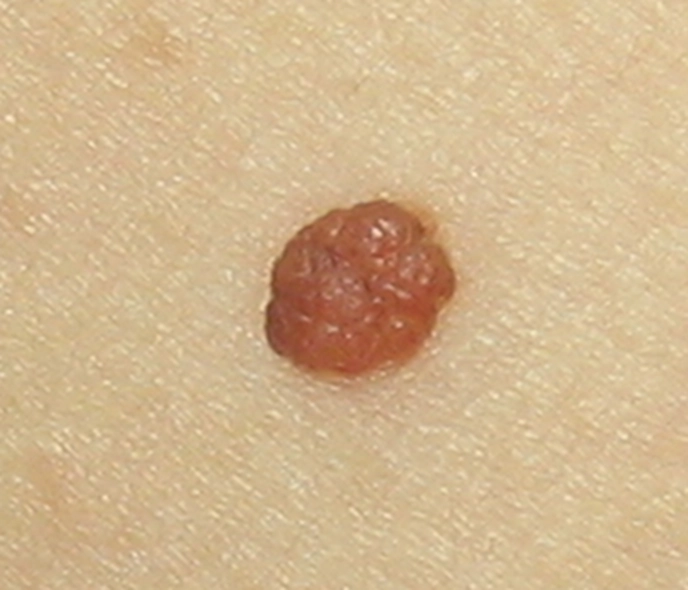
- Compound melanocytic naevi are raised brown bumps, most of which are hairy. Some have a slightly warty surface.
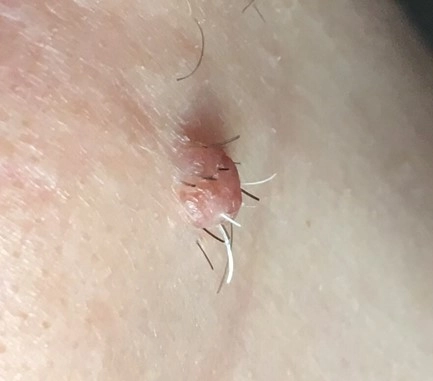
- Intradermal melanocytic naevi are raised, often hairy, bumps, like compound naevi, but paler in colour (they often have no pigment).
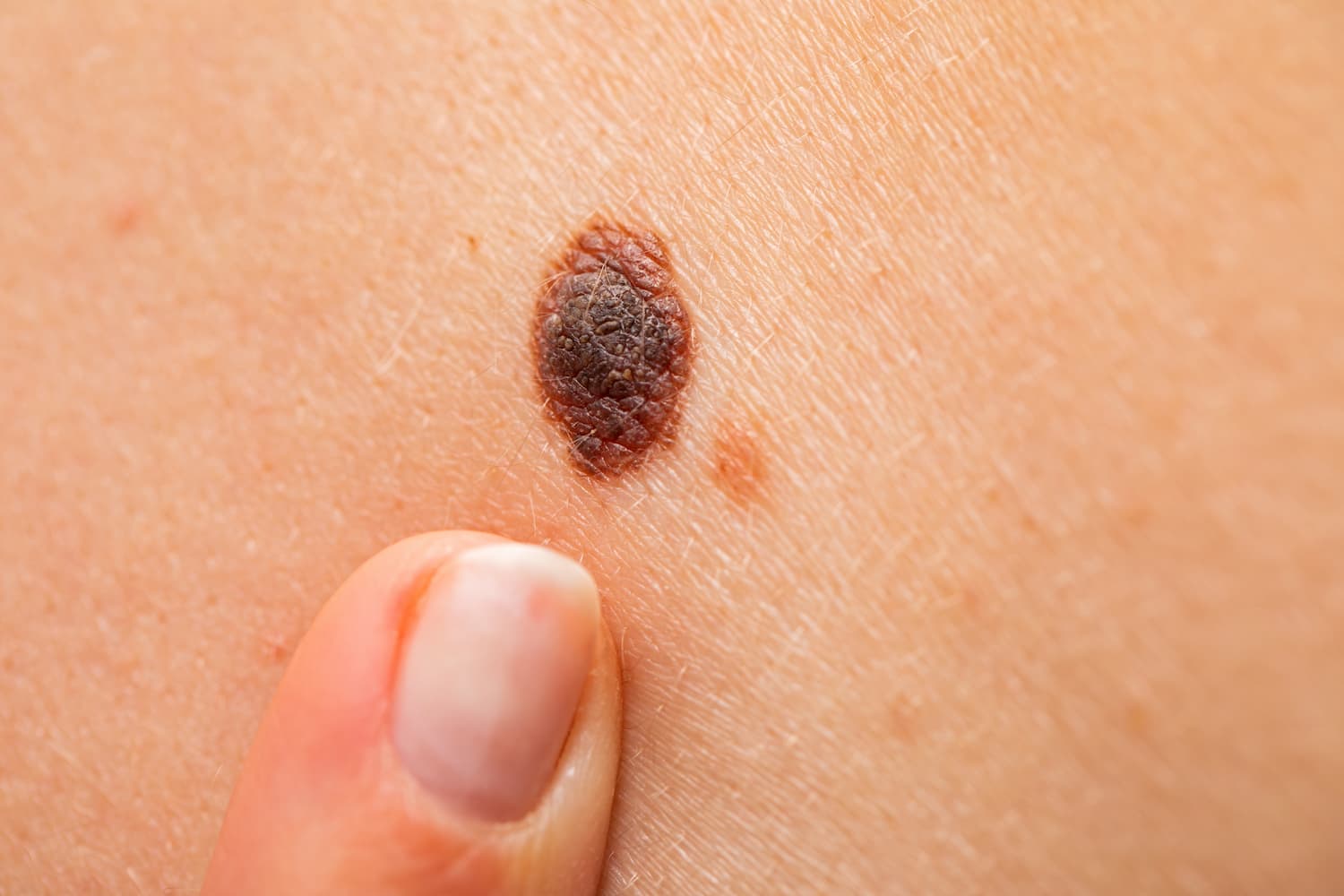
Three common types of melanocytic naevi:
In childhood, most moles are of the junctional type. Later in life some become raised and hairier, and moles on the face often become pale over time.
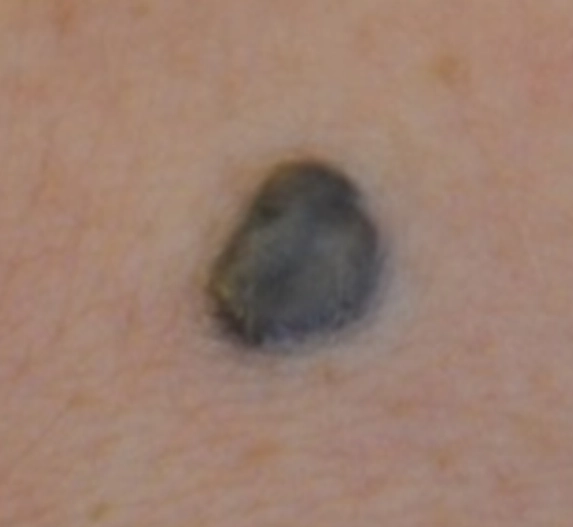
Less common types of melanocytic naevi:
There are several other, less common, types of mole. These include:
- Blue naevus - a harmless mole with a dark blue colour.
- Halo naevus - a mole surrounded by a pale ring which may gradually go away by itself.
- Dysplastic or atypical naevi’ - these are usually multiple, with irregular pigmentation and shape, and run in some families. They have a greater tendency than most moles to change into a melanoma, which is a skin cancer.
How are melanocytic naevi diagnosed?
Most melanocytic naevi can be recognised easily by their clinical appearance. If there is any concern over the diagnosis, particularly over the possibility of a melanoma (see below), your doctor will arrange for the mole to be removed and checked in the laboratory. It may occasionally be difficult to diagnose a mole from a seborrhoeic keratosis (a harmless dark warty mark that is common in older people).
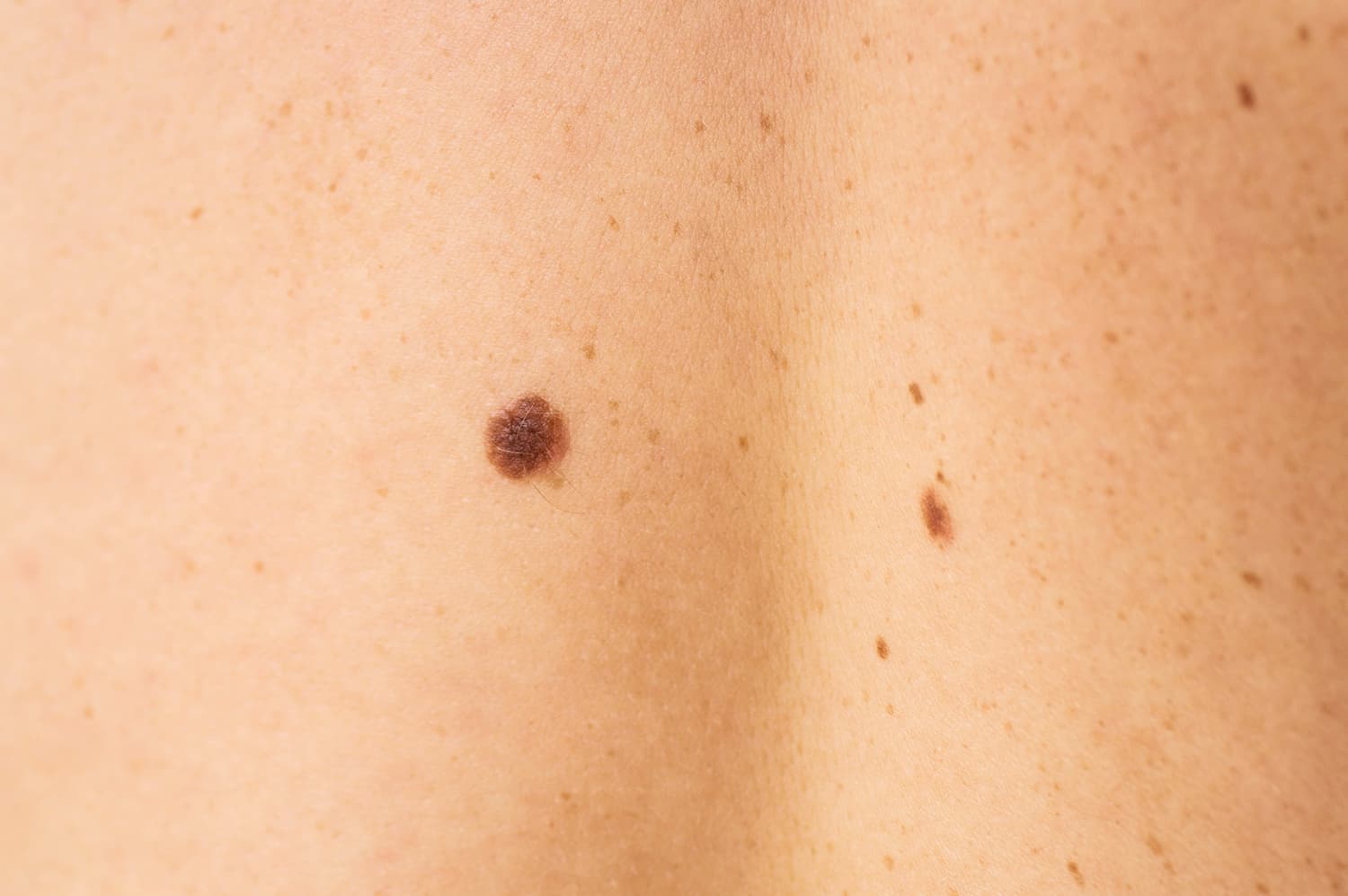
What are the worrying signs to look out for?
The risk of a mole changing into a skin cancer called melanoma is very small but it is important to have them properly diagnosed because melanoma is a serious type of skin cancer. Up to two thirds of melanoma are new pigmented lesions and one third develop from pre-existing moles. We commonly look for loss of symmetry of a mole, changes to the border, changes in colour, an increase in size above 6mm, and a history of evolving change in a pigmented lesion.
Do you know the ABCDEs of melanoma?
Early detection is essential for melanoma, the most dangerous type of skin cancer.
Here's what to look for:





Treatments for melanocytic naevi
Benign melanocytic naevi do not need removing unless there is a history of significant change or an assessment by a specialist advises that removal is necessary on medical grounds. Moles can be removed for personal cosmetic reasons, but this is not funded in the NHS. Some types of moles especially pigmented moles on the face are best left alone as the scars can look worse than the original mole.
Surgical options for treatment
Shave excision
Benign raised moles can be safely removed by a specialist using this technique. This is most effective for moles that are skin coloured or not too dark in colour. This is a simple procedure that requires a small injection of local anaesthetic and use of a specialist blade. The skin heals like a graze over 7-12 days. This often produces normal skin or a flat white mark. Occasionally, the skin can be red for several weeks after treatment. Some moles will regrow or re-pigment with time, but the procedure can be repeated.
This involves removing the entire mole and some surrounding skin after injection of a local anaesthetic. This involves external stitches and the procedure typically takes about 20-30 minutes. Cosmetically, this will produce a linear or straight-line scar that may stretch to become a white scar longer-term.
Other complications of surgery include wound infection, bruising, disturbance to the skin sensation, and rarely a raised red scar called a keloid scar. The appearance of the skin after surgery may look worse than the original mole so we do not normally recommend routine removal unless there is a medical indication.
Ellipse excision
Self-care (What can I do?)
If you have many moles:
- You should examine your skin monthly for moles that are growing or changing in the ways described above. If you find any worrying changes or a mole that is clearly different from the rest, it is advised to contact your doctor immediately. It is normal for moles to appear up until age 30-40; a new mole after this age should be regarded with more suspicion.
- You must also protect yourself from too much sun exposure. This does not mean that you cannot ever go on a sunny holiday again; it just means that you need to be careful to avoid sunbathing and burning. You should cover yourself up and use sun protection creams of SPF 30 or above (see the ‘top sun safety tips’ below for more information). Do not use sunbeds.
- Protect your skin with adequate clothing, and do not forget to wear a hat that protects your face, neck and ears, and a pair of UV protective sunglasses. Choose sun protective clothing (with permanently sun-protective fabric, widely available for adults and children) if you have fair skin or many moles.
- Spend time in the shade between 11am and 3pm when it’s sunny. Step out of the sun before your skin has a chance to redden or burn.
- When choosing a sunscreen look for a high protection SPF (SPF 30 or more) to protect against UVB, and the UVA circle logo and/or 4 or 5 UVA stars to protect against UVA. Apply plenty of sunscreen 15 to 30 minutes before going out in the sun and reapply every two hours and straight after swimming and towel-drying.
- Keep babies and young children out of direct sunlight.
- The British Association of Dermatologists recommends that you tell your doctor about any changes to a mole or patch of skin. If your GP is concerned about your skin, you are advised to see a Consultant Dermatologist – an expert in diagnosing skin cancer. Your doctor can refer you for free through the NHS.
- Sunscreens should not be used as an alternative to clothing and shade, rather they offer additional protection. No sunscreen will provide 100% protection.
- It may be worth taking Vitamin D supplement tablets (available from health food stores) as strictly avoiding sunlight can reduce Vitamin D levels.
Vitamin D advice
The evidence relating to the health effects of serum Vitamin D levels, sunlight exposure and Vitamin D intake remains inconclusive. Avoiding all sunlight exposure if you suffer from light sensitivity, or to reduce the risk of melanoma and other skin cancers, may be associated with Vitamin D deficiency.
Individuals avoiding all sun exposure should consider having their serum Vitamin D measured. If levels are reduced or deficient, they may wish to consider taking supplementary vitamin D3, 10-25 micrograms per day, and increasing their intake of foods high in Vitamin D such as oily fish, eggs, meat, fortified margarines and cereals. Vitamin D3 supplements are widely available from health food shops.
Where can I get more information about melanocytic naevi?
Web links to detailed leaflets: www.dermnetnz.org/lesions